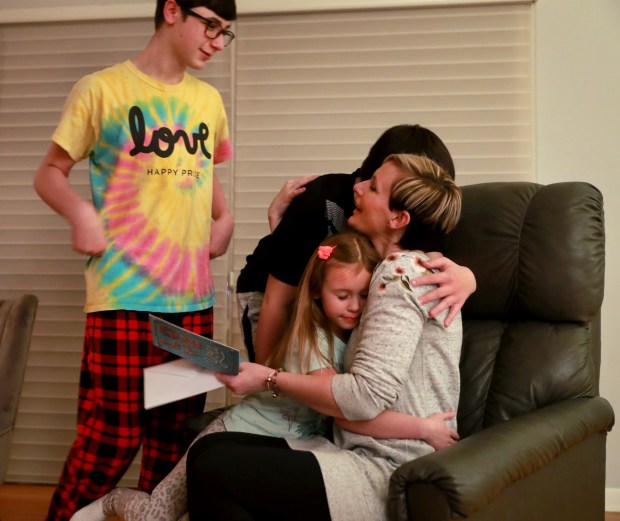After a year of undergoing treatments to fight off an aggressive form of breast cancer, Heather Mingay was scheduled to have her ovaries removed this month, in an attempt to help prevent the cancer from returning.
Mingay, 37, of Northbrook, told her manager at work she’d be gone. She secured extra child care for her three kids. She mentally prepared.
And then her doctor’s office called her about 21/2 weeks ago to cancel the surgery. The call came as hospitals across the state suspended elective procedures to help keep beds open, amid a nasty COVID-19 surge that’s sent many people to hospitals, especially the unvaccinated.
“I could cry right now,” Mingay said, shortly after learning her procedure was postponed. She’s now cancer-free and wants to stay that way. “This is not elective. It’s not a choice, but I have to kind of sit on the sidelines right now, and the longer I sit on the sidelines, my risk goes up for recurrence.”

It’s no secret that the current wave of COVID-19 has sent case numbers soaring and filled hospitals across Illinois. But over the last couple of months, it has also made it difficult for people with problems that aren’t immediately life-threatening to get medical care.
Patients in need of certain non-emergency surgeries, such as Mingay, have seen those surgeries postponed. Though many of the delayed surgeries are called “elective” they are actually necessary, though not emergency, procedures. Long ER waits have also become common for patients with serious but non-life-threatening illnesses and injuries. And urgent care centers are increasingly turning patients away for hours, days or even weeks at a time because they’re short on staff and overwhelmed with demand.
“No matter where you’re going to go right now in health care, you’re probably going to experience a delay,” said Dr. Richard Freeman, Loyola Medicine regional chief clinical officer.
Stacey Fanale, 53, of Geneva, saw that firsthand after a sharp pain under her ribs jolted her awake in the middle of the night in late November.
Her husband drove her to the nearest emergency room, at Northwestern Medicine Delnor Hospital in Geneva.
But it was the beginning of the current COVID-19 surge, and the ER was so backed up that Fanale had to wait about five hours to be seen, after a nurse determined that her condition wasn’t life-threatening. She lay on a couch near the waiting room, in searing pain, until after sunrise. Ultimately, she had to have her gallbladder removed that day.
“I was in excruciating pain, but the nurse was like, ‘This is the way it is,'” said Fanale, noting that she doesn’t blame the doctors and nurses for the wait, but rather the latest COVID-19 surge and how it’s been handled.
She wonders why, after nearly two years of the pandemic, hospitals, businesses and governments haven’t come up with a better plan for providing medical care through surges.
“COVID is a part of today’s world. This cannot continue,” Fanale said. “All of us need to come up with a solution to move forward so that everybody has medical care.”

Chris King, a spokesman for Northwestern Medicine, acknowledged in a statement that ER wait times are longer than usual across Northwestern’s hospitals, though he noted that the problem is not unique to Northwestern.
Doctors at other Chicago-area hospitals have described ER wait times of up to eight hours in recent weeks.
Several factors are to blame.
For one, hospitals are short on staff, amid nationwide labor shortages. Burned out by the pandemic, many health care workers left their jobs in the last two years, and those who remained are now often having to stay home for days at a time because they caught COVID-19. Even vaccinated people are getting COVID-19 during this wave, though they’re typically not getting as sick as people who are unvaccinated.
Secondly, there’s the latest COVID-19 surge itself, which has set records for case numbers and hospitalizations.
The result is that hospitals can’t staff as many beds as they need for patients, which is why Gov. J.B. Pritzker urged hospitals across the state to postpone elective surgeries. It’s also meant that an increasing number of patients who need to stay overnight in hospitals must wait in beds in emergency rooms until beds open up elsewhere in the hospital — a practice that can back up ERs, leading to longer waits for patients as they arrive.
“You’re trying to take a higher volume of patients for a lower number of beds, and it makes for, unfortunately, much longer wait times than any of us want,” said Freeman, with Loyola.
The situation at urgent care centers, which are facing similar challenges, isn’t helping matters in emergency rooms.
Traditionally, urgent care centers have been touted as an alternative to emergency rooms for patients with pressing but non-life-threatening health needs. But over the last couple of months, a number of Chicago-area urgent care centers have been turning away patients because of staff shortages and overwhelming demand.
In recent months, NorthShore University HealthSystem’s urgent care centers have sometimes been closing hours early to new patients because all of their patient slots fill early in the day. This week, UChicago Medicine Ingalls Memorial Hospital’s Flossmoor Urgent Aid location reopened after closing for weeks because of strain from this latest COVID-19 surge.
Closures of urgent care centers have become common across the country during this COVID-19 surge, said Lou Ellen Horwitz, CEO of the Batavia-based Urgent Care Association. In the northeastern part of the country, about 20% of urgent care centers temporarily closed at one point, at the peak of COVID-19 there.
“That’s a big deal for most communities,” Horwitz said. “It definitely has a trickle-down effect to other health care providers.”
Jerry Zielinski, 74, of Downers Grove, tried to go to an Advocate Health Care immediate care center near his home earlier this month, after he slipped on ice in his driveway while trying to get the newspaper. He fell hard, hitting his head and back on the ground.
But when he and his wife arrived at the urgent care center, they were told it didn’t have the staff that day to take X-rays or perform CT scans. Instead, the urgent care center directed Zielinski to Advocate Good Samaritan Hospital.
Once there, he waited in a crowded ER, wondering if any of the people sitting near him had COVID-19. In pain, he spent more than five hours shifting uncomfortably in a waiting room chair. He learned that he had two broken ribs but no concussion.
“There’s care we as regular people need and it’s been proven to be difficult to get because of the frequency and severity of COVID,” Zielinski said.
In a statement, Advocate Good Samaritan Hospital said, “The COVID-19 surge and national staffing crisis are straining health systems, and it has resulted in full beds and long wait times,” and apologized for resulting inconveniences.
Horwitz, with the Urgent Care Association, said many urgent care centers are trying to address the overload with tactics such as only performing COVID-19 tests by appointment, so they can keep their walk-in slots available for people with other types of medical needs. Some are trying to keep slots open by only performing COVID-19 tests for people with symptoms of the illness, rather than those who were merely exposed.
Horwitz is hopeful that new federal programs to give people free at-home COVID-19 tests, through a website and health insurance companies, will also take some of the pressure off of urgent care centers.
Doctors and hospital leaders also say there are things that can be done to potentially help avoid ER backups and cancellations of elective surgeries in the future — but some of those things will take time to accomplish. Already, the state and federal governments have sent additional staff to Illinois hospitals in recent weeks to help out, but doctors say they need more people to go into health care in coming years.

More needs to be done to support front-line health care workers, such as through pay, affordable child care and student loan forgiveness, said Dr. Joseph Sakran, director of emergency general surgery at The Johns Hopkins Hospital in Baltimore, who’s written about how this surge has affected care. And investments must be made to build up state and local public health infrastructure to better respond to disasters and pandemics, he said.
In the past, when a region experienced a crisis, such as a hurricane, the federal government stepped in and filled in the gaps. “But when the federal government is asked essentially to respond to the entire nation, it’s not just one small location or one small region, then you’re able to see we weren’t prepared to do this.”
In the short term, one of the most important things people can do is to get vaccinated, health care leaders say. Though vaccinated people can still catch COVID-19, they don’t typically need hospitalization. Fewer people needing hospitalization could mean shorter ER waits and a return to performing all elective surgeries.
Mingay, who is still waiting for her surgery, is eager for that day. She is now hoping to have her procedure in the coming months, barring another bad COVID-19 surge. She’d like to see everyone do their part, by masking and getting vaccinated, so this doesn’t happen again.
“Mentally, it’s like being on this roller coaster,” Mingay said. “It just keeps going.”